Videos you might be interested in
Videos you might be interested in
Videos you might be interested in
Suggested for you
No Breast Milk After Delivery: Reasons and Diagnosis
It could take up to half a week after delivery before any milk is available in a mother's breast. Certain medical complications and medical birthing procedures can delay the onset of lactation. It has also been noted that up to twenty-five percent of all mothers may experience a delay in lactation of more than three days. This, however, does not mean that lactation will not set in, but it can be a cause for concern. Read on to understand about delayed lactation, its possible causes, and remedies.
What Triggers Breast Milk to Come in?
Prolactin, Cortisol, Oxytocin and Insulin are hormones that are essential for the production of breast milk, and are generated in a woman’s body throughout her pregnancy. The production of breast milk, however, is only triggered 30 to 40 hours after birth. The hormone progesterone, which inhibits the production of breast milk, drops after the baby is born and the placenta separates from the uterus. This reduction in progesterone triggers the production of breast milk.
When Does Breast Milk Come in After Delivery?
A couple of days after delivery, the mother's breast begin to feel full; this is the first sign that her milk is coming in. Prolactin, a hormone that signals the mother's body to produce milk, rises throughout the duration of the pregnancy. The effects, however, are negated by the production of another hormone, progesterone. This is produced by the placenta, which inhibits the body from effectively responding to prolactin. The normal production and supply of breast milk in the mother's body only begins when the baby is born, and the hormones of the placenta have left the mothers body. Pregnant women observe that sometimes their breasts are leaking a little milk. Colostrum is the rich, creamy first milk that a woman's breasts start producing from mid-pregnancy. This will provide the necessary nourishment to the newborn before breast milk comes in.
Causes of No Breast-milk
Natural breastfeeding is considered to be the best option for newborn babies. For some mothers, unfortunately, this may not be possible, at least early on. There are a multitude of reasons why breast milk may not come in or is produced in very low quantities. Unable to fulfil the baby's requirements, it is also a contentious issue among experts and medical practitioners. Here, we will highlight some of these reasons and try to understand the underlying causes of no breast milk.
1.Stress
Our hectic modern day lives, leave us with less time and less contact with family, friends, and sometimes, with the aspirations and emotional needs of the self. Stress is identified by medical practitioners as one of the core reasons for a myriad of ailments. This includes anxiety, heart disease, depression, and lack of breast milk production. Stress can cause the body to act and react in unexplainable ways.
2. Hormonal Imbalances
Often described as a small butterfly-shaped organ, the thyroid gland, though tiny, is crucial to maintaining a balance of hormones. A malfunctioning thyroid gland will cause hormonal imbalances, resulting in low or no milk production. Among the important hormones, oestrogen and progesterone are associated with breast development, puberty and the onset of fertility in women. Prolactin aids in milk production during pregnancy and Oxytocin helps with the flow of milk through the ducts. The lack of these hormones on account of thyroid gland function or any other factor will interfere with the production of breast milk.
3. Lifestyle
Pregnancy is a delicate phase. Much care and attention have to be paid to the lifestyle choices made during this time. A sedentary lifestyle, improper diet, indulgence in alcohol, drugs, habitual smoking, and high caffeine intake can impact the production of breast milk.
4. Birth Control
Most birth control medications work by manipulating the hormones in the body. These artificially applied manipulations may cause consequences, both in the short-term and long-term health of women. Some women start taking medications after the baby is born and this practice could result in no milk production after delivery.
5. Taking Certain Medications And Herbs
Like birth control medications, certain other medicines and some herbs can interfere with the production of breast milk. Consult your doctor about prescription medicines or any other medicines that you take regularly. Herbs such as sage, oregano, parsley and peppermint are all known to inhibit breast milk production. It is advisable to consult medical practitioners and experts on the diet best suited for breast milk production.
6. Environment And Surroundings
Increasing air pollution, contamination of water and food, and environmental degradation are the harsh realities of modern life. Such factors may also interfere with the production of breast milk. While not much can be done to completely shield yourself from this reality, certain precautions in terms of food and water can certainly be undertaken. It would also be prudent for women with breastfeeding babies to avoid overcrowded and polluted places for a while.
7. Difficult Delivery
Even with knowledge, skill and technology at our disposal, things don't always go as planned. This holds true with pregnancy as well. There are numerous issues you could face while delivering a baby. From difficult labour and haemorrhage to mistakes by caregivers and medical staff, many factors can lead to a traumatic delivery. The stress caused by such delivery may impact the production of breast milk. Post partum hemorrhage after deliverycan lead to acute decrease in hormone levels and no milk production, called Sheehan's Syndrome.
8. Storage Size
The amount of milk produced and stored in a woman's breast is not related to the size of the breasts themselves, but the amount of milk-producing tissue in them. Some women may have large breasts and a small capacity, and in some women, the reverse may be true. Sometimes, one side of the breast may produce more milk than the other. Women whose breasts produce and store more milk will have to feed or pump out milk more often.
9. Insufficient Draining of Milk
In an ideal setting, the more a baby breastfeeds, the more the mother's body will produce milk. If the baby is not able to breastfeed properly, the leftover milk will not allow the breasts to produce more milk. It is necessary that the breasts are drained of milk to initiate more milk production. Massaging the breasts can aid more milk to flow and ensuring that the baby is able to latch on properly will help proper draining of milk.
Delayed Onset of Lactation
Under normal circumstances, colostrum is available in the mother's breast within 40 hours of delivery. Breast milk generally takes two-three days to arrive. In some cases, breast milk may take up to five days to arrive. ‘Delayed onset of lactation’ is the term applied to a condition wherein the breast milk is slow to come in. A delay in the production of breast milk does not mean it will not arrive at all. Some medical birthing procedures and medications could be possible reasons for the delay. Some likely causes for delayed onset of lactation are listed below.
1. Stressful Delivery
C sections and prolonged labour may increase stress hormones, directly affecting the production of breast milk.
2. IV Fluids
Administration of IV fluids during birth could delay the onset of lactation.
3. Blood Loss
The pituitary gland can be damaged in the event of excessive blood loss during delivery. This gland, located in the brain, is responsible for triggering lactation. A blood loss of more than 500 ml is a cause for concern.
4. Placenta
Remnants of the placenta can trigger the release of progesterone, which prevents the onset of lactation.
5. Painkillers
Pain relief medications, if administered during labour, can delay the onset of lactation.
6. Premature Birth
Glandular tissue in a mother's breast does not have sufficient time to develop in case of premature birth, which could delay the breast milk coming in.
7. Breastfeeding
It is crucial to breastfeed or hand express milk within the first couple of hours after birth. Hand expressing or breastfeeding in the initial days after birth is necessary, as new milk will not be produced until the old milk is out.
8. Diabetes
One of the important hormones for breast milk production is insulin. Diabetes causes fluctuation in insulin levels, which can delay the onset of lactation.
9. Age
Giving birth at an advanced age could also be a reason for the delayed onset of lactation.
10. Anxiety
Stress, fear and insecurity arising from delayed onset of lactation can further complicate matters and result in breastfeeding no milk coming out.
What to Do If Breast Milk is Not Coming in or Coming Late?
In case breast milk is not coming after delivery, you should not get upset or disappointed. Doing so will only raise stress hormones further complicating this condition. Hand expressing every couple of hours could stimulate milk production, and hence, should be done. It is also advisable to consult doctors and be open to formula milk or donor human milk till the onset of lactation.
Tips to Quicken Lactation
1. Hand Express Breast Milk
Even if you don’t get any milk, hand express regularly. This will trigger lactation, allowing your breast milk to come in sooner.
2. Massage Your Breasts
Massage your breasts in a circular, downward motion. The pressure can help bring in your breast milk sooner.
3. Increase Skin to Skin Contact
Skin to skin contact, where you hold the baby close to you, and let his skin rub against yours, is known to stimulate the production of milk. This has helped many new moms lactate quicker.
4.Avoid Taking Any Medications
Avoid taking any medications for any other health issues, without your doctor’s approval, as some are known to decrease or delay the production of breast milk.
5. Consult Your Doctor
Don’t run to your doctor at the first instance. Wait for a while and let your body naturally begin its lactation process. If it doesn't occur, then consult your doctor to check if there are any factors hindering breast milk production.
Breastfeeding is part of nature's beautiful design to create a bond between mother and child. Breast milk not coming in at all is extremely rare and highly unlikely. It is advised to consult doctors and lactation specialists to address the condition. Above all, it is essential that moms take care of themselves, both physically and emotionally.
Also read: Breast Pain During Pregnancy: Causes, Effects & Remedies
References and Resources: Mayoclinic Read more
Suggested for you
10 Rainy Day Essentials for Children
Children go berserk when the first rains hit the grounds and, before you know they will be out on the streets, screaming and shouting, and playing around in the rain. You find out about it only when they return back home, drenched, and sniffling or even sneezing. Children and rain are inseparable, which is why one of the important ways to keep them safe is to have children's rain gear in place as well as keep a bunch of other tips in mind.
Video: 9 Rainy Day Essentials for Children
https://www.youtube.com/watch?v=s4FRLnQV0qY
Monsoon Essentials for Kids
Here are some rainy-season essentials for your kids:
1. The Trusty Umbrella
This is the first thing you ought to go out and buy when the signs of rain start becoming imminent. An umbrella is quite good at providing a basic level of protection from the rain and can help you move around and reach a safer place, too. Get your kid one for his size in his favourite colour or one that sports his favourite cartoon.
2. The Fully-Covered Raincoat
Torrential rains and speeding vehicles can make umbrellas useless, as water seems to come from every direction. Especially when kids are returning from schools, their uniform and bags can easily get wet. Purchase a nice bright coloured raincoat that is full-sized and covers your child from head to toe. Go for separate shirt and pants pieces if needed. If it can cover their bag as well, that’s an added bonus.
3. The Right Footwear
Having proper footwear is essential for your child since he will tend to walk through pools of water and dirty areas whenever he steps outside or is returning home. Keeping the feet clean is essential as well as getting shoes that prevent slipping or skidding on the road. If you stay in an area of torrential rainfall, invest in gum boots as well.
4. A Portable Sanitizing Option
You might take effective care of your child at home, making sure he washes his hands properly. But at school, the same cannot be always ensured. If he plays around during recess and ends up having lunch without washing his hands properly with soap, you are in for a ton of problems, especially in the monsoons. Get him a small sanitizer which he can keep in his bag. Insist on washing hands but let him know that he can quickly clean them with a few drops from the sanitizer as well.
5. A Warm Jacket Can Be Quite Useful
Protection from rain while outside is necessary. But protection from cold weather is a necessity, too. At times, constant rain can bring down the temperature instantly, making your child feel cold at home. A nice warm jacket can prevent him from getting cold or contracting a fever. If you can get a raincoat that functions as a warm jacket, which will keep him warm even when he’s drenched.
6. Utilize Towels that Absorb Well and Dry Quick
Your child might get wet multiple times in the day, necessitating a proper bath frequently. This makes it necessary to have a towel that can clean the body well, absorb all the water, as well as dry quickly to be used again. Invest in such a towel, especially for your kid, so that he stays dry at all times. Get a small napkin as well that he can carry around in his school bag.
7. Water-Proof Carry Bags are Helpful in Various Ways
Carrying out wet umbrellas and raincoats can be quite a pain. Or carrying something extra in rain without the right way to protect it can pose a challenge. Having a few carry bags in your child’s schoolbag can resolve the problem. These need to be waterproof so as to prevent anything inside them from getting wet, as well as stop water inside them from seeping outside.
8. Wet Wipes Can Help Clean Things Up Real Quick
With monsoons come inevitable slip-ups and mud splotches on the body and the clothes. It may not always be possible to find a tap and clean it all quickly. Having a small box of wet wipes helps remove the dirt quickly and dispose of them in the dustbin right away. If water has splashed all over the child, he can wipe his face to keep himself clean and then reach home quickly to clean the rest.
9. Extra Clothes Can Be Carried Too
If your child is going to be away from home for longer durations, such as at school or a day-long picnic, it is best to give him a change of clothes. Getting wet in the rain and being stuck without a change can expose him to contracting a cold and fever quite easily. A change of clothes can keep him dry at all times.
10. Safe and Healthy Snacks to Munch on
This requires some participation from your child as well. Rather than give him money to eat food outside, give him healthy snacks to keep in his bag instead. Advise him to stay away from street food and give him tasty alternatives instead. Keep them with you, too, when stepping outside with your kid.
Kids love monsoons. And they love to go wild and have a fun time with their friends. No matter where they are, taking a few steps to keep them safe can go a long way in ensuring that they can continue being the fun-filled kids they are and enjoy the rains to their fullest.
Also Read: Monsoon Activities for Children Read more
Suggested for you
Blocked Tear Duct in Babies
From yellow discharge to eye infections, blocked tear ducts cause discomfort to babies and worry to parents. Tears cannot drain properly when the duct is blocked, and the duct ends up swelling or getting infected. Keep reading to learn more about blocked tear duct in babies.
What is a Blocked Tear Duct?
A blocked tear duct is a condition when the tear duct (where tears drain through a small tube in the eyes) gets blocked or doesn't open up properly. Blocked tear ducts usually reveal themselves during the first two weeks after the baby is born, when the baby starts getting "watery" eyes. A yellow or white discharge often accompanies them, and sometimes this discharge ends up sealing the eyelids shut too.
How Common is it in Babies?
Almost 6 out of 100 newborns are affected by blocked tear ducts after birth. They may occur during the baby's birth year and may not cause any eye problems when they first appear as well.
Causes of Blocked Tear Duct
The common causes of a blocked tear duct in infants are-
When the tissue at the end of the tear duct is not able to open up
Eye infections
When the nasal bone grows abnormally, thus putting pressure on the tear duct and sealing it off
Partial or underdeveloped openings near the corners of the eyes where the tears drain out
Signs and Symptoms of Baby Blocked Tear Duct
Symptoms of a blocked tear duct usually appear during the first few days to weeks after being born.
Yellow or white discharge from the corners of the eyes
Redness and swelling of the eyes
"Watery" eyes
Tears streaming down the cheek
Epiphora (excessive tearing)
Tenderness or a bump near the side of the nose
Swollen blue bump near the inside corner of the eyes (also known as dacryocystocele)
Eye infections accompanied by fever, mucus or pus in the eyes
Diagnosis and Tests
Most blocked tear duct conditions in babies resolve naturally with time. However, sometimes a little bit of testing and diagnosis never hurts to cross-check if it spurs from underlying causes. The following three tests are used for diagnosing a blocked tear duct -
Tear Drainage Test- A special dye is applied to your child's eyes to check whether or not tears drain correctly. If the duct has anything that is blocking its path, then the dye remains on the eye's surface even after 5 minutes pass.
X-Ray Exam - An X-ray or CT scan of the dacryocystogram (tear duct area) is done to check for blocked tear ducts. It is followed up with an MRI to image the location of the blockage and identify its causes.
Medical Evaluation - Your doctor may evaluate your medical history to ascertain whether tear duct blockages run in the family. A physical examination and an ophthalmic examination are done to check for other plausible reasons for blockage.
How to Treat a Blocked Tear Duct in Your Child?
Blocked tear ducts usually open up on their own. Meanwhile, here are 6 treatments you can try to help them open up and get those tears draining-
1. Surgical Probing - Surgical probing is a procedure done at the hospital to manually open up the tear ducts through surgery. It's done on an outpatient basis, and your ophthalmologist will recommend it if your baby has a severe infection and must be admitted to the hospital. The procedure lasts for about 10 minutes.
2. Silicone Tube Intubation - Silicon tubes are inserted into tear ducts to stretch and open them up. The tubes are kept in place for 6 months and surgically removed afterwards.
3. Balloon Catheter Dilation (DCP) - A balloon is placed into the tear duct by insertion through the corner of the eyes and inflated using a sterile solution to expand the tear duct openings. It is afterwards deflated and removed from the eyes.
4. Antibiotic Eye Drops - If an infection spreads, your baby's paediatrician may prescribe your little one some antibiotic eye drops or eye ointment. These drops or ointments aid in clearing up infections and eliminate harmful bacteria from blocked tear ducts.
5. Chinese Medicine - Chinese medicines are useful and effective for treating conjunctivitis or "pink eye" conditions. Herbs like Ju Hua also treat allergy-related tear duct conditions.
6. Aloe - Use a little amount of aloe from the inside of an aloe leaf and rub that gently on both the eyelids to reduce swelling and redness.
Home Remedies for Baby's Blocked Tear Duct
Home remedies work just as well as surgical treatment. Try these before you consider surgical procedures for your little one-
1. Breast Milk - Apply a few drops of breast milk to treat blocked tear ducts in your little one's eyes and watch them recover gradually.
2. Tear Duct Massage - Ask your doctor to demonstrate how to do a massage to help your baby's blocked tear duct and be gentle. Basically, you apply gentle pressure between the tear ducts along the upper nose area to aid in clearing up the ducts. This can be done up to two times a day, every day.
3. Warm Compress - Take a soft, clean washcloth and dip it in warm water. Gently wipe the insides of the duct and work your way outward so that particles don't enter the eye. If both your baby's ducts are blocked, you must use another clean washcloth or a cotton ball to repeat the process.
Prevention
Prevention is better than cure. Here are some ways you can prevent your baby's tear duct from facing blockage in the first place-
Wash your hands- Before and after cleaning their eyes, make sure to wash your hands and maintain hygiene.
Massage regularly - You don't need to massage your baby's tear ducts only when there's a blocked tear duct. By massaging from the start, you'll prevent those tear ducts from clogging beforehand.
Environmental Factors - Reduce exposure to sunlight, cold, and wind for your infant to prevent tear duct blockage.
Wipe Their Eyes - Use small cotton balls or a clean cloth to wipe away any excess drainage from your baby's eyes regularly, especially the outer parts.
A blocked tear duct is nothing serious or extreme to worry about. It happens to many babies and the above remedies will certainly come in handy. Try these out and watch them heal soon!
Also Read: Remedies for Pink Eyes in Babies Read more
Suggested for you
Epidural Anaesthesia During Labour- Risks and Benefits
As D- day approaches, every mom finds herself wondering 'how painfulis labour?'. Labour is surely painful , however thanks to modern medical science, we now have several medication and techniques that can reduce (if not stop) pain during labour and delivery.
Epidural anaesthesia is a popular and safe method of pain relief during labour. Opting for an epidural indicates having a small amount of medicine injected in the body to produce desirable pain relief. However, like all medicines, it is important that you understand the benefits and risks involved in epidural, so that you can make an informed choice well before getting into labour.
What is an Epidural?
An epidural is a local anaesthetic that aims to provide pain relief or an analgesic effect, rather than a total lack of feeling (anaesthesia). It blocks the nerve signals from both motor and sensory nerves to reach your brain. It shields you from pain while immobilising your lower body while allowing you to stay conscious during labour. Epidural can be used for both vaginal (normal) and a caesarean delivery.
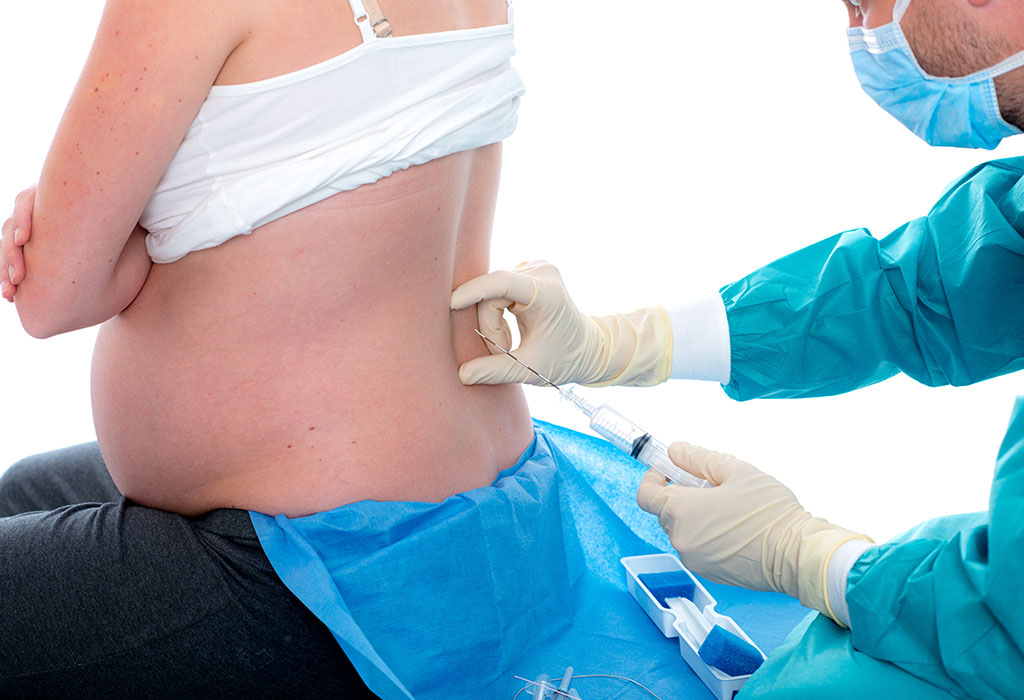
Epidural anaesthesia during labour is administered on your lower back into a small space (also called epidural space) outside the spinal cord through a hollow needle or a catheter. A catheter allows for repeat or continuous delivery of the anaesthetic medication, when needed. An epidural injection for pregnancy is designed to provide partial pain relief for women, however, the decision to opt for it is entirely up to you.
Types of Epidurals
While hospitals and anaesthesiologists differ on the dosage and combinations of medication, there are broadly three type of epidurals that are used during labour.
Traditional/ Standard Epidurals
Apart from the regular use of a cathedar, traditional epidural uses regular anaesthesia medications such as bupivacaine or lidocaine that eliminates pain to a great extent. It is injected around the spine creates a heavy feeling and numbs the lower body. Therefore, mothers find it difficult to move during labour. However, you will still be able to move with some help in walking or moving.
Spinal Epidurals/ Spinal Block
Unlike a traditional epidural, spinal epidural involves the anaesthesia being injected into the spinal cord fluid directly. This gives faster relief from the labour pain but the effect of the drug wears off after a few hours. Spinal blocks are generally used late in labour. Spinal epidural once administered also makes body movements limited.
Walking Epidural or Combined Spinal Epidural (CSE)
This is a combination of drugs, local anaesthetic medication and epinephrine. Unlike other epidurals, CSE allows you to have slight sensation in your lower body. Hence, mobility is not much of an issue in this case. The advantage of maintaining some mobility in spite of the motor block, potentially helps in getting the baby into a better position for faster delivery.
How is an Epidural Injection Administered?
An epidural injection is usually given during the 'active' stage of labour by an anaesthesiologist or gynaecologist. You will be asked to sit at the edge of the bed, bend your back and remain steady. This position is important for preventing any complications and thereby increasing the effectiveness of your epidural medications. Another favourable position to do so is to lie on one side, bend and curl your knees to as high as you can possibly bring them. Both of these allow a good spinal curve to assess the exact location where the injection must be administered.
An antiseptic solution is applied on your skin to eradicate any chances of infection. A small area on your back is made numb by local anaesthesia administered through an injection. A needle is then directed into the area surrounding the spinal cord in your back followed by a catheter through the needle into the epidural space. The anaesthesiologist then carefully removes the needle, leaving the catheter in its place, in order to give medication as per requirement. The catheter is then safely taped on to the back to maintain its position.
Once you are through with the above procedure, there are a few ways to administer an epidural that can be adopted. All these methods are crucial to determine the amount of medicine that needs to be administered for an effective pain relief depending on your threshold and condition:
1. Epidural using a catheter: A catheter (a bendable thin and hollow tube) is put in carefully into the epidural space created by using a hollow needle. This allows the continuous or intermittent administration of medication just outside the membrane surrounding your spinal cord and spinal fluid. Your anaesthetist will first give you a "test dose" to check the placement of the catheter tube and check for any adverse drug reactions. If you do not develop any reactions, the test dose is followed by a full dose.
2. Intermittent Epidural: In this case, the medicine is given on a need basis. Based on your tolerance level for the labour pain and desired level of movement your anaesthesiologist will decide the dose .
3. Mix and Match: The anaesthesiologist mixes medicines (anaesthetics and analgesics) to match the degree of sensation and movement you want.
4. Patient-Controlled Epidural Anaesthesia: With the help of this epidural, you can regulate the amount of medication injected into the epidural tubing.
5. New Epidural Births: Also called as “walking epidurals,” this particular analgesia gives the mother freedom to stand, kneel, squat, or even walk with some help.
6. Spinal Analgesia: The newest pain reliever is known as spinal analgesia or a “walking spinal.” Only a tiny dosage of medicine is injected into the spinal fluid to reduce the agony of labour but still allows movement.
7. Low-Dose Epidurals: This is a type of combination (narco-anaesthetic) epidurals. They are designed to relieve some of the pain of labour so that an exhausted mother can relax a little and get some energy back for pushing.
How Does an Epidural Anaesthesia Work?
An epidural temporarily blocks the nerves in your cervix and uterus that carry pain signals to your brain and thereby decrease the sensation.
Epidural medications include drugs called local anaesthetics, such as bupivacaine, chloroprocaine or lidocaine. They are usually given with opioids or narcotics so that local anaesthetics can be used less.
This produces pain relief with less side effects. Such medicines may also be used to prolong the epidural’s effect or to stabilize the mother’s blood pressure.
What is the Right Time to Have an Epidural?
There is no right or wrong time to have an epidural analgesia during labour. However, it is usually given during the active stage of labour, when you feel more frequent contractions and your cervix has dilated.
You may also be offered an epidural if your labour has to be sped up. This is done with a hormone called Syntocinon, administered in a drip which make your contractions more intense and painful.
The epidural has to remain in its place until after your baby is born . It can also provide pain relief after delivery if you need stitches from an episiotomy.
Advantages of Having an Epidural
Epidurals are a great choice to relieve labour pain better than any other medication. Women who have been administered epidural feel very less or no pain durimng labour. Other advantages are:
It does not significantly increase duration of labour.
You can stay awake and alert but you will still feel the pressure and some stretching during delivery.
Combined spinal-epidural (CSE) gives better results than does a standard epidural. It has lower doses of anaesthetic medications that give you more muscle strength.
It‘s strength can be enhanced with a local anaesthetic if needed. Though having an epidural does not increase your chances of needing a caesarean.
Possible Disadvantages of Taking an Epidural
An epidural can be used to deliver different types of local anaesthetics, which also differ in the side effects that they cause. Common epidural side effects include
Itching : If that happens, changing the drug may help in solving the problem.
Drop in blood pressure and fever : Even a small dose of epidural may cause a drop in blood pressure or induce fever. However, this is normal.
Numbness or tingling sensation in the legs : This can create difficulties in urinating. A urinary catheter is normally used in such cases to help you urinate.
Risk of spinal fluid leak: If the injection goes too deep, it can make a hole in the protective layers (dura) around the spinal cord, and spinal fluid might leak out. This may result in headaches that can last up to days. This can happen due to fluid loss.
Longer duration of childbirth: Delivery may take a bit longer on an average amongst women who have epidurals.
Assited delivery: Some women may feel the desire to push in spite of having an epidural. Due to the epidural they cannot feel when it is time to push, they may need assisted delivery (vacuum suction/forceps)
Does Epidural Have Any Side Effects on Baby?
In general, epidurals are safe for the baby as it is injected into the spine and not through veins. Any medication that is given to a woman during her labour surely reaches the baby’s bloodstream through the umbilical cord. This includes pain-relieving anaesthetics delivered through epidurals. But anaesthetics use drugs that are as safe as any other painkillers that are given to expectant mothers and hence do not affect the baby strongly. There aren’t any long term side effects of using epidurals.
However, since the babies’ immune system is weak, it takes more time for them to remove epidural drugs. Similarly a drop in the blood pressure of the mother due to epidural, may cause discomfort to the baby as it may affect his oxygen supply.
Is Epidural Birth Painless?
Parents have fear and anxieties involving labour pain and childbirth. Having an epidural does reduce pain, however doesn't eliminate it completely.
On an average epidural takes about 40 minutes to work after it is injected. The process of administrating it is painful and can be quite uncomfortable. If the same medicine is used in lower concentration, it will cause analgesia which means it will only relieve the pain without causing any muscle weakness. However, if the epidural does not work, your doctor may have to administer it again.
Taking an epidural will provide some pain relief however, a 'painless delivery' is not entirely possible.
Can the Use of an Epidural Injection Cause Back Pain in the future?
Even after going thorugh childbirth with the help of an epidural, some women may experience mild soreness at the catheter site where the medication was injected. Using an epidural pain relief during delivery does not cause long-term back pain. While many women believe that epidural analgesia causes severe or long-term back pain, they are not related. Back pain post-delivery happens due to the pre-existing prenatal backaches or are a result of normal physiological changes during pregnancy.
Epidural and Multiple (twin) Pregnancy
It is not necessary to have a caesarean delivery with twins. Just like a single child delivery, many twins are born vaginally too. Epidurals are often recommended by doctors for pain relief in labour and also in preparation to get the second child in position for delivery.
If there are any problems, it's practically easier for your antenatal team to deliver your babies quickly if you've already had an epidural.
What Happens After Delivery?
It's important to focus on your baby's birth during pregnancy. But it's a good idea to also know what to expect after labour.
The umbilical cord is clamped and cut, and your baby is dried and covered up to prevent catching cold.
Mucus is cleared out of your baby’s face. Some babies need assistance to get their breathing normal.
Bonding starts with skin-to-skin contact. Hold your baby close to you.
Your baby will be examined by a paediatrician, weighed and measured, and given a band with your name on.
Once your precious bundle of joy is born, the toughest journey of your pregnancy may be over, but the process of care bringing him up will always continue. Your body starts to recover and you learn to adjust to the new role of motherhood. Read more
Suggested for you
Suggested for you
Rashmi has added a new answer
Guardian of 0 children
19 hours ago
Q. #asktheexpert hi this is Sarika here . my question is how to encourage my baby to latch because he get irritated whenever I try to latch him

Rashmi
Mom of a 9 yr 7 m old girl
19 hours ago
A. It’s very important that when you ask a question please provide us the age of the child currently I would say that if your child is unable to latch properly so whenever you’re feeding Press your breast with your hands for the feeding of the milk is better because the milk flow is going to be better and hopefully that you do the trick
Mohammad amin has added a new answer
Guardian of 0 children
8 hours ago
Q. my baby have gastric problem..

Mohammad amin
Guardian of a 2 yr 11 m old boy
7 hours ago
A. use colimex df drops
Rashmi has added a new answer
Expecting Mom due in 1 month
8 hours ago
Q. #asktheexperts red scretch marks

Rashmi
Mom of a 9 yr 7 m old girl
8 hours ago
A. You can mix coconut oil and Kapoor together and that is what you can apply regularly want to your stretch marks is one of the best options that you can use currently other than that also I would recommend you that if you feel any kind of a burning sensation or irritation then you can have a word with your gynaecologist
Dr Vandan H Kumar has added a new answer
Guardian of 0 children
4 hours ago
Q. left side pain kyu hota h

Dr Vandan H Kumar
Paediatrician
4 hours ago
A. many times and the most common cause would be due to accumulation of milk clots and sometimes it can be neurogenic pain and sometimes it might be a partx any local mass like lymph nodes or tissue pain.
if it is not improving with simple massage as well as simple hot compressesx and expression of accumulated milk then meet your doctor at the earliest for local examination.
you can take paracetamol for pain.
Sai Prasanthi R L has added a new answer
Expecting Mom due in 7 months
3 hours ago
Q. I got chicken pox in my 8th week..it's just started how I can deal with it?

Sai Prasanthi R L
Mom of a 10 yr 2 m old boy
3 hours ago
A. Hello dear! Chicken pox during pregnancy is a matter of concern. Consult your doctor for personal evaluation and seek medical advice. Maintain a good personal hygiene routine and follow your doctor’s advice. Good luck and take care
Dr Laxmi Chavan-Sawant has added a new answer
Guardian of 0 children
2 hours ago
Q. is sesame seeds healthy in 37th week of pregnancy

Dr Laxmi Chavan-Sawant
Ayurvedic Gynaecologist
54 mins ago
A. yes you can have but limited .
During pregnancy it is always advisable to have your normal routine foods and include more of sprouted grains along with green leafy vegetables and adequate water intake which helps maintain good health
Do have regular daily walking
Check out this new Memory

Sindhu Krishna
Mom of a 3 yr 8 m old girl
New Memory
#cutestbaby

0 Likes
0 Comment
Check out this new Memory

Parul
Guardian of a 7 yr 1 m old girl
New Memory
#cutestbaby

0 Likes
0 Comment
Check out this new Memory

parvathy
Guardian of a 6 m old girl
1 min ago
My ima baby.

0 Likes
0 Comment
Check out this new Memory

patel falguni
Guardian of a 5 yr 6 m old girl
2 mins ago
#risingstar

0 Likes
0 Comment
Check out this new Memory

Aparna Ch
Mom of a 6 m old boy
3 mins ago
#posterbaby

0 Likes
0 Comment
Tell us more about yourself get More Personalised
 Infant0 to 6 Months
Infant0 to 6 Months Baby6 Months to 2 Yrs
Baby6 Months to 2 Yrs Toddler2 to 4 yrs
Toddler2 to 4 yrs Kids4-6 yrs
Kids4-6 yrs Big Kids6+ yrs
Big Kids6+ yrs Expecting
Expecting Trying to Conceive
Trying to Conceive




.svg)
.svg)
.png)